During the COVID-19 pandemic, hospitals around the world leaned heavily on single-use personal protective equipment (PPE). It was a crucial line of defence to keep patients and healthcare workers safe. But now that the dust has settled, we are beginning to understand the environmental toll it took. Mountains of used PPE ended up in landfills, incinerators, or worst case in the natural environment. Plastic pollution soared, and the carbon footprint of healthcare spiked noticeably. What kept us safe in the moment has left a lasting mark on the planet.
But as the saying goes, never waste a good crisis. The pandemic didn’t just expose the environmental cost of disposable PPE, it also revealed how fragile global supply chains really are. Hospitals around the world scrambled to secure enough gowns, masks, and gloves amid skyrocketing demand. It was a wake-up call. Now is the time to rethink our approach. Reusable protective equipment has proven to be just as safe, more cost-effective, and far less harmful to the environment. It also makes healthcare systems more resilient in the face of future disruptions. As health systems look for ways to cut their carbon emissions, switching to reusable PPE is a practical, high-impact step in the right direction.
Environmental Impacts: What the Science Says
So, what kind of difference can reusable PPE actually make? Beyond the common-sense appeal, there’s now solid research backing up the environmental benefits of reusables. From gowns to masks, studies consistently show that switching to reusable protective gear can dramatically reduce emissions, plastic waste, and resource use without compromising safety or hygiene. Let’s break it down.
Life Cycle Assessment studies comparing reusable and disposable PPE consistently find that reusable alternatives offer a significantly lower environmental footprint. Take surgical and isolation gowns, for example: switching from disposable to reusable versions can cut greenhouse gas emissions by up to 66% and reduce solid waste by as much as 84%, even when accounting for the energy and water used for laundering.
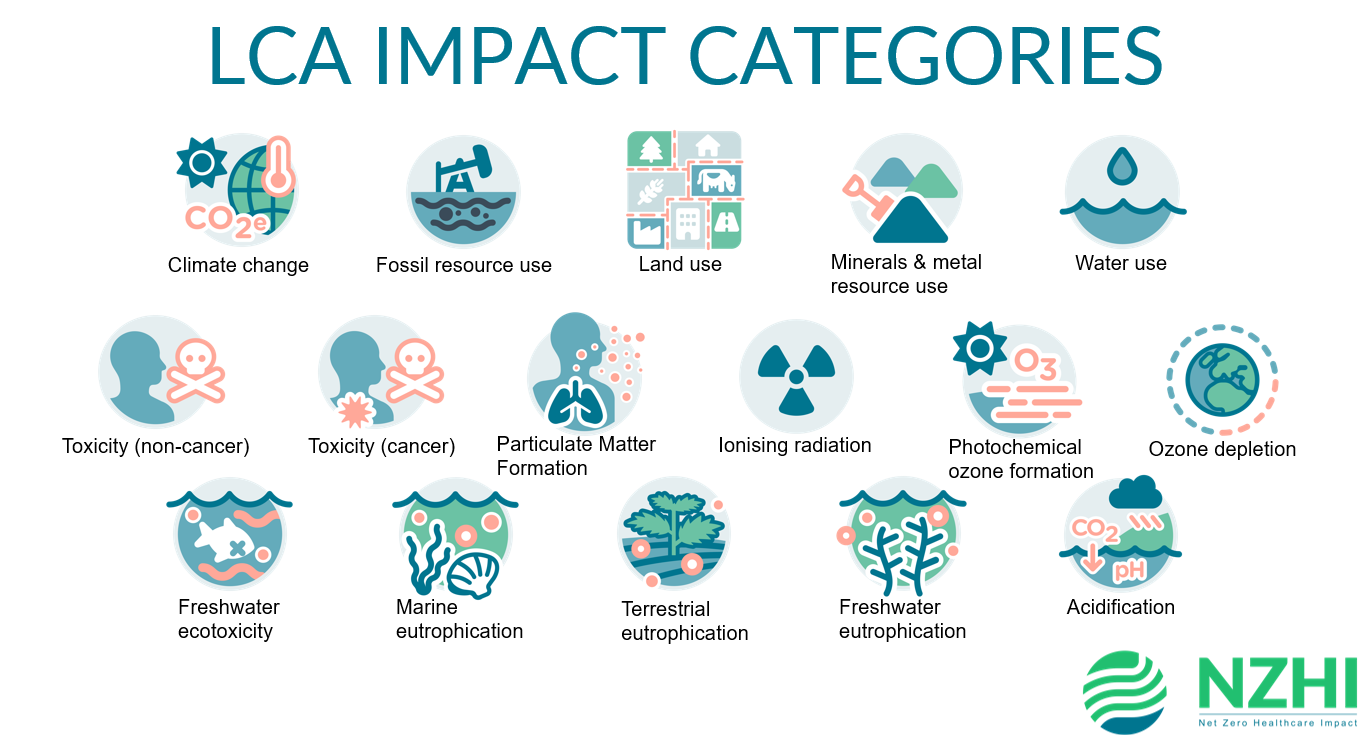
Figure 1: Overview of the 16 LCA impact categories.
Face masks tell a similar story. The World Health Organization estimated that during the COVID-19 pandemic, approximately 52 billion disposable masks were used in 2020 alone. This resulted in over 5,000 tonnes of plastic ending up in the oceans and roughly 1.1 million tonnes of CO₂e emissions. Most of that footprint came from raw material extraction, packaging, and manufacturing.
Also, disposable scrubs and coveralls would benefit from a rethink. A study¹ found that reusable scrub suits are better for the environment across nearly every metric: they use less energy and water, emit fewer greenhouse gases, and require fewer harmful chemicals. Although laundering contributes to their environmental footprint, when done in energy-efficient or renewable-powered facilities, the overall impact of reusable workwear drops significantly. In fact, the carbon footprint of a scrub top can be reduced by more than 70%.
Then there are body coveralls, often worn in high-risk settings. The disposable kind, typically made from melt-blown polypropylene, can persist in landfills for decades and contribute to microplastic pollution. When comparing disposable and reusable versions, studies² show that although reusables require more water for washing, they outperform disposables on nearly every other environmental front, from lower emissions to reduced toxicity.
Even gloves present opportunities to reduce environmental impact. While there is currently no reusable alternative for medical gloves, smarter usage can still make a meaningful difference. One study³ found that sterile surgical gloves have over 11 times the climate impact of non-sterile ones, primarily due to the energy-intensive sterilization process. In procedures where sterility isn’t essential, switching to non-sterile gloves can significantly lower emissions. By matching glove type to actual clinical risk, hospitals can reduce waste without compromising safety. Just as importantly, reducing unnecessary glove use altogether can have a major impact. Wearing gloves only when clinically indicated not only cuts waste but also aligns with best practices in infection prevention. Re-evaluating when and why gloves are used can challenge ingrained habits and lead to more sustainable care, without compromising patient or staff safety.
 Figure 2: Visualization of gloves consumed in a single day in medical emergency department.
Figure 2: Visualization of gloves consumed in a single day in medical emergency department.
Safe, Comfortable, and Staff-Approved
Of course, safety is non-negotiable in healthcare. The good news? Reusable protective gear doesn’t compromise on it. When properly cleaned and maintained, it performs just as well as its single-use counterparts. Independent studies confirm that reusable gowns, masks, and scrubs meet the same high standards for protection, breathability, and durability. For example, the widely used ANSI/AAMI PB70 standard applies equally to both disposable and reusable PPE.
Staff preferences also play an important role in success. The University of Antwerp performed acceptability studies for reusable PPE amongst healthcare staff and found that the acceptance was immediately very high for gowns, caps and aprons. Within a period of 3 months, almost full acceptance was achieved and this should be considered as a transition period where both options are provided. Only for masks it took longer to accept the reusable PPE, probably because of the intimacy of the mouth. At Massachusetts General Hospital, a large-scale shift to reusable scrub caps was a clear success. Not only did the switch reduce waste, but 86% of clinicians reported preferring the reusable caps over the bouffant disposables. Staff cited better comfort and fit, and having names embroidered on the caps improved compliance and reduced mix-ups.
Figure 3: Reusable Personal Protective Equipment.
The Business Case for Reusable PPE
In a cost-conscious sector like healthcare, price matters. And while disposable PPEs might seem cheaper at first glance, the full picture tells a different story. When factoring in the entire lifecycle (incl. purchase cost, frequency of use, laundering, and eventual disposal) reusable PPE often comes out ahead. Not only is it better for the environment, but it can also deliver significant long-term savings. One case study makes this clear: switching to reusable gowns led to a 30% cost reduction compared to disposable alternatives, even before accounting for savings on waste handling or compliance with waste regulations.
Coveralls have a similar story. Even when laundering is taken into account, reusable versions are more cost-effective over time, especially when you include the hidden costs of constant reordering and treating disposables as hazardous waste. Reusable scrub caps are another smart investment. At Massachusetts General Hospital, staff loved the personalized caps, but financially they made sense too. The hospital broke even within 15 to 26 weeks, depending on how often they were washed. So, it’s fair to say: reusable PPEs don’t just save the planet, they save money too.
Coveralls have a similar story. Even when laundering is considered, reusable versions are more cost-effective over time, especially when factoring in the hidden costs of constant reordering and the disposal of single-use gear as hazardous waste. Reusable scrub caps are another smart investment. At Massachusetts General Hospital, staff appreciated the personalized caps, but they made financial sense too. The hospital broke even within 15 to 26 weeks, depending on laundering frequency. So, it’s fair to say: reusable PPEs don’t just save the planet, they save money too.
Boosting resilience
Reusable systems not only reduce costs but also enhance supply chain resilience, a factor that becomes critical during high-demand crises such as pandemics. Countries like Austria, which had already adopted reusable PPE systems by 2020, fared significantly better during the COVID-19 pandemic than many other European countries whose hospitals depended heavily on single-use PPE imports from Asia. When the pandemic hit, a severe mismatch between supply and demand occurred, and many hospitals and governments ran into serious shortages.
Figure 4: PPE from European textile producers such as Alsico.
A key factor in the increased resilience of reusable PPE is that many of the reusable textiles are produced by European textile producers such as Alsico and Vetex and local laundries do the washing. For hospitals it’s important to include ’surge capacity clauses‘ in the contracts with textile producers and laundries. This provides the possibility for a dramatic increase in output during crisis situations such as pandemics or geopolitical events in which the supply to the healthcare industry becomes a critical bottle neck. PPE should be considered a critical good and reusable PPE should be an essential part of strategic autonomy and business continuation plans by both local, national and European governments and by the hospitals and healthcare providers.
Smarter Storage, Longer Life: Managing PPE More Sustainably
All PPE, whether single-use or reusable, comes with a defined shelf life. For disposables, it reflects how long the material retains key properties like filtration or barrier strength. For reusables, it also includes durability across washing cycles. Proper storage helps PPE reach that lifespan. Keep items in cool, dry, and dark conditions, away from sunlight, humidity, or temperature swings. Leave packaging sealed until use. Use first in first out (FIFO) stock rotation and digital inventory systems to avoid early waste. Reusables should be stored clean and dry, ideally in breathable textile bags or sealed boxes to prevent degradation.
By law, only manufacturers can officially extend shelf life. But during crises, governments may authorize the use of expired PPE after quality tests by certified labs. In the U.S., the CDC allows expired PPE in low-risk settings after inspection. Non-clinical uses, like for cleaning teams and visitors, are also safe fallback options.

Figure 5: Smart storage of PPE.
Smart End-of-Life Solutions for PPE
For personal protective equipment (PPE) that has exceeded its official shelf life and is no longer fit for clinical use or was used in non-hazardous settings, several sustainable end-of-life pathways are emerging. These strategies reduce waste and promote circular material flows. One option is mechanical recycling: plastics found in surgical or FFP2 masks can be shredded and processed into granulate for new products like storage boxes or pallets. Other studies showed that mixed polymers from FFP2 masks can be repurposed without complex separation. Other research highlights the use of shredded PPE as an additive in concrete, improving its mechanical properties.
Chemical recycling offers more advanced options. Polypropylene from masks can be transformed into high-value raw materials or activated carbon. Social or creative upcycling can repurpose PPE into tote bags or insulation materials, providing opportunities for social enterprises and community-initiatives. Lastly, thermal valorisation remains the most commonly applied pathway, where the waste is incinerated for energy recovery, partially replacing fossil fuels.
From Linear Waste to Circular Value
Reusable PPE isn’t just good for the planet, it’s also good for people and prices, and thus comprises the triple bottom line. Hospitals are among the largest institutional users of textiles and plastics, so switching to reusables is a powerful, evidence-based way to cut waste, lower emissions, build resilience, and save money. It aligns perfectly with broader goals like the EU’s Green Deal and the carbon neutrality targets many hospitals are working toward. By integrating reusable PPE into sustainability roadmaps, hospitals can move from linear, waste-heavy consumption models to circular systems that prioritize reuse, durability, and local economic development.
But making the switch is not as simple as swapping one product for another, it requires strategic planning. First and foremost, laundering is critical. Whether managed on-site or through a certified third-party provider, facilities must meet strict hygiene standards and use energy- and water-efficient systems to unlock the full environmental benefit. Furthermore, procurement teams should also prioritize quality and durability. Reusable garments built to last, with features like reinforced stitching and robust closures, make a significant difference in both safety and longevity. Equally important is staff engagement. Involving clinical teams early, and providing clear guidance on how to use, clean, and replace reusable PPE, helps ensure a smooth and successful transition.
In the end, moving to reusable PPE is a smart way to reduce emissions, cut costs, and build resilience without compromising safety or comfort. But it won’t happen by accident. Successful hospitals typically start with a simple step: conducting a (PPE-)waste audit to understand current usage and disposal patterns. From there, pilot programs can help staff become familiar with the change. Then, procurement and operations teams can step in to source durable gear and set up reliable laundry infrastructure. With the right approach, reusable PPE isn’t just an environmental win, it’s a practical pathway to stronger, leaner, and future-ready healthcare.
At NZHI, we help hospitals turn sustainability goals into measurable impact.
Whether you're launching a targeted pilot, embedding sustainable PPE into an existing strategy, or building a comprehensive sustainability roadmap from scratch, NZHI supports you every step of the way. Our science-based tools and hands-on expertise ensure your efforts are not only effective, but also cost-efficient and aligned with your broader goals. Let us help you move from intent to impact.
References:
- Mikusinska, 2012, Comparative Life Cycle Assessment of Surgical Scrub Suits, The Case of Reusable and Disposable Scrubs used in Swedish Healthcare
- Snigdha et al., 2023, Environmental footprints of disposable and reusable personal protective equipment ‒ a product life cycle approach for body coveralls
- Jamal et al., 2021, Non-sterile examination gloves and sterile surgical gloves: which are more sustainable?
- Ravagen et al., 2023, Comparative Environmental Impact Evaluation of Disposable Surgical and Reusable Cloth Face Masks
- Crespo et al., 2021, Study of Recycling Potential of FFP2 Face Masks and Characterization of the Plastic Mix-Material Obtained. A Way of Reducing Waste in Times of Covid-19
